Osteochondral Allograft Transplantation (OCA)
A fresh graft of cartilage and bone can be transplanted from a cadaver to fill in a cartilage (and bone) defect. The donor cells live in the recipient. There are no drugs to take and no rejection occurs.
What it is:
The implantation of a graft of cartilage and bone from a cadaver. Derives from the Greek words for bone (osteo), cartilage (chondral), and allo (other/different person). It is usually taken from a cadaver knee for implantation into the knee of a patient, but can apply to other joints as well.
What it is used for:
The femur (thigh bone) has “condyles” at the end of the bone within the knee. These condyles are bone covered with cartilage. If the cartilage and/or bone are diseased, pain results. OCA implants healthy cartilage and bone into the diseased area.
How the procedure is performed:
Part of a donor knee is brought into the operating room. This cadaveric knee must not be more than 30 days old. A graft from the donor knee is fashioned to fit into the defect in the patient’s knee. Coring reamers are used to size-match the graft so that it can be press-fit into the defect.
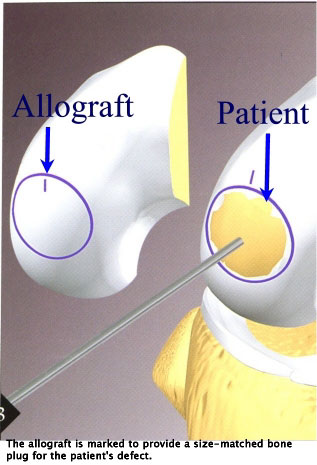
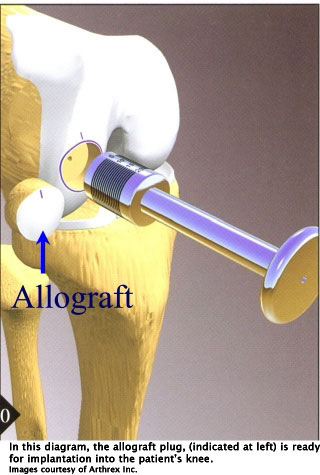
Incidence of rejection:
Cartilage is not rejected and drugs are not needed.
Incidence of disease transmission:
This can occur, although the incidence is extremely low. Estimates range from one in 30,000 to one in a million; only a few cases have been reported. Bacteria and viruses, such as HIV and hepatitis can be transmitted.
Waiting period:
A donor is usually found within a few weeks.
Risks of the procedure:
Infection can occur about 1% of the time. Incomplete pain relief can occur as well as implantation failure requiring further surgery. Stiffness requiring surgical removal of scar tissue occurs rarely. Blood clots, RSD (chronic pain syndrome), and other rare complications can also occur.
Post-surgical regimen:
The patient usually can go home the day after surgery, non-weight bearing for the first two weeks. The patient will become progressively partial weight bearing, using crutches or a walker.
Alternatives to the OCA:
These can include bracing, medication, injections, articular cartilage implantation, microfracture, unicompartmental knee arthroplasty and total knee arthroplasty.









