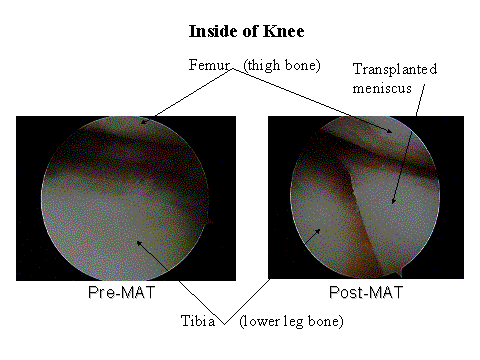
Meniscal Allograft Transplantation (MAT)
If the cushion-like meniscus of the knee has previously been surgically removed, the knee can prematurely degenerate. In many cases a meniscus from a cadaver can be transplanted to help arrest the deterioration of the knee and relieve pain. The success rate of this procedure for properly selected patients is 85-90%.
What it is:
The surgical insertion of a human cadaveric meniscus into a meniscus-deficient knee.
Definition of meniscus:
A fibrocartilaginous structure that cushions the joint surface. In the human knee there are two: a medial or inner, and lateral or outer.
What happens after a torn meniscus is removed from an injured knee:
If it is partially removed there is usually no effect. If most or all of it is removed, however, pain and degeneration may develop over time.
Length of time for symptoms to develop after the meniscus has been removed:
Usually several years. In some patients pain and degeneration never develop after meniscectomy.
How meniscal allograft transplantation helps a previously meniscectomized knee in pain:
It provides restored “cushioning”. The transplantation relieves pain and appears to inhibit the progression of arthritic changes in the joint.
Limitations on the procedure:
There are some knees that are too severely affected to benefit from meniscal transplantation. If the joint space is severely reduced between the bones, indicating advanced arthritis, meniscal allograft transplantation is unlikely to provide lasting benefit.
Type of procedure:
It is performed primarily arthroscopically with two additional small incisions. It may be performed on an outpatient basis, but most patients stay overnight in the hospital and go home the day after surgery.
Surgery notes:
The meniscus is inserted in the knee through a small incision. A piece of bone attached to the meniscus from the cadaver is attached to the bony bed in the knee of the patient. The meniscus is then sutured into the tissue of the patient’s knee.
Risk of infection:
It is possible, but the risk is very small. Recently a few infections occurred from transplanted tissue, but this was traced to improper procedures from a tissue bank that is no longer being used. Overall, the safety record has been exceedingly good over many years and many thousands of procedures.
Risk of tissue rejection:
There is none. The transplanted meniscus is a nonliving tissue from a human donor and does not cause rejection the way a living transplant such as a heart or kidney does. No anti-rejection medicines are needed.
Other risks:
Stiffness occurs occasionally. This may require a separate procedure to remove scar tissue from the knee to regain motion. Other rare complications may include, but are not limited to, nerve damage, reflex sympathetic dystrophy and chronic pain.
Effectiveness of the meniscal transplantation:
In properly selected patients the success rate is 85-90%. Some patients will need repeat arthroscopy to trim the transplanted meniscus.
Walking after the procedure:
You can walk on the day of surgery. You will be given crutches and will be partial weight bearing immediately.
Resumption of athletic activities:
You will usually be able to resume unrestricted vigorous activities within six months.
Insurance coverage:
In almost all cases where it is needed, insurance will pay for the procedure.
Case Histories
Go to our case histories for patient #1 and patient #3 to read about patients who had meniscal allograft transplantation surgery done along with other procedures.