Patient #8 – 24 year old man with a history of ACL reconstruction and recent damage to the knee
About the Patient
This 24 year-old man had torn his left ACL as a teenager and had it surgically reconstructed. The graft used for the surgery was an allograft. Also during the surgery, a medial meniscectomy and a lateral meniscal repair were performed. After recovering from this initial surgery, the knee functioned fine, until the patient slipped and fell, damaging the knee again.
When he was seen in our office, he complained of pain and had moderate swelling in the knee. KT1000 testing showed mild laxity in the damaged knee suggesting a partial re-tearing of the ACL. Conservative treatment of physical therapy was tried, but the symptoms of pain continued to worsen. An MRI showed cartilage damage and a possible tear in the medial meniscus.
Treatment
Surgery was performed with plans to access the damage to the ACL graft and deal with the cartilage and meniscal damage.
The ACL graft showed a partial tear. The anterior (front) part of the graft had torn and a lump of torn graft was present at the base of the ACL graft. The remaining posterior (back) part of the graft did not appear to have integrated well with the surrounding tissue. The graft appeared to be separate from the surrounding tissue and did not show ingrowth of that tissue. All of the loose, damaged tissue was removed. Then small holes were drilled into the areas around the graft (similar to a microfracture) until the areas bled freely. This was done to create a healing response to help the surrounding tissue integrate with the remaining ACL graft.
Both the lateral and medial menisci were examined. The medial meniscus had mostly been removed during the previous surgery. The remaining rim was stable and nothing was done. The lateral meniscus showed a small tear. However, the tissue was also stable, so nothing was done here either.
The cartilage that covers part of the femur was examined and there was found to be an area where the cartilage was damaged and bone was exposed. This area was about 5.5mm in size and was surrounded by an area of partial thickness damage. The loose tissue was trimmed away from the area and a microfracture was performed in the area where the bone was exposed.
See the pictures and video at the bottom of the page to see the images of the damaged ACL graft and cartilage.
Results
Because of the microfracture, the patient was partial weight-bearing for the first 6 weeks after surgery. After that he began physical therapy which continued for 4 months. During this time his knee continued to improve. By 1 year after the surgery, the patient had full range of motion in the leg and was pain free. He continued to have a mildly more lax left knee due to the partial tear of the ACL graft, but this did not affect his ability function.
About 20 months after the surgery, the patient returned to the office. After running on the knee, he developed pain and swelling again in the knee. The MRI did not show any problems. Suspecting either another meniscal problem or a failure of the microfracture, surgery was scheduled.
Second Surgery
The second surgery revealed that the previously stable lateral meniscal tear had expanded and now was unstable. The location of the tear correlated with the location of the pain the patient was experiencing. A lateral meniscectomy was performed to remove the unstable area.
The surgery also offered an opportunity to take a second look at both the ACL graft and the site of the microfracture. The ACL graft showed a good healing response to the stimulation applied during the previous surgery. The graft was covered with healthy tissue and was integrating with the surrounding tissue. The graft also appeared thicker than it had previously. The microfracture site showed healthy tissue covering the entire area. The tissue was probed and found to be healthy and well-attached.
The pictures and video below show the before and after images of the ACL graft and the microfracture.
Results
Although this patient is still recovering from his most recent surgery, he is doing well and is expected to recover and be pain free again. He will continue to have mild instability because of the partially torn ACL, but should be able to function well.
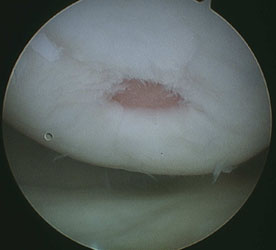
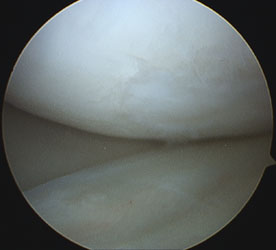
The left image shows the damaged cartilage. The red area is exposed bone. Fissures of damaged cartilage radiate from this area. The right area shows the same area 22 months later. The area that was originally damaged is completely filled with fibrocartilage and the fissures and other damage around the site have also filled with tissue.
The video on the right shows the ACL graft. First is shown the graft at the initial surgery. At this time, it is partially torn with debris from the tear present and poor integration with the surrounding tissue. At the end is shown the graft at the time of the second surgery. At this point, the graft is showing smooth integration with the surrounding tissue.









